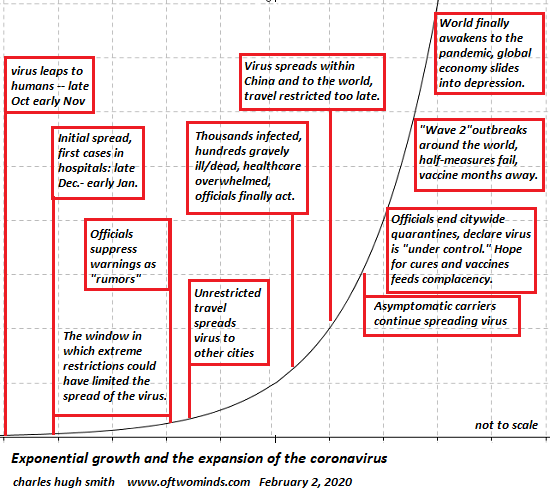
Either the science is wrong and the complacent will be proven correct, or the science is correct and the complacent will be wrong.
The present disconnect between the science of Covid-19 and the status quo’s complacency is truly crazy-making, as we face a binary situation: either the science is correct and all the complacent are wrong, or the science is false and all the complacent are correct that the virus is no big deal and nothing to fret about.
Complacency is ubiquitous: readers on Facebook leave comments on my posts “this is silly.” Correspondents report that people don’t even cover their mouths when coughing, much less use a tissue. People keep repeating like a mantra that a bad flu season kills 35,000 in the U.S. alone, and so why worry about a couple thousand deaths globally?
Another common trope is “hepatitis kills far more people in the U.S., so why worry about the coronavirus?”
So let’s look at some data and consider what science can tell us about the potential consequences of the Covid-19 virus spreading as widely as conventional flu viruses.
The fallacy made by the complacent is that the number of cases will remain small (in the dozens or hundreds) and so the number of deaths will also remain small.
Since the evidence suggests the Covid-19 virus is more contagious than conventional flu viruses, a reasonable assumption is that it will eventually infect more people than a conventional flu, which according to the CDC infects up to 45 million Americans annually.
According to the CDC, viral hepatitis B caused 5,600 deaths in the U.S. in 2017, and hepatitis C caused 19,000 deaths, for a total of 24,600. That certainly exceeds reported deaths of Covid-19, but since the statistics presented by the Chinese government are unreliable, we have no idea how many people have the virus and how many have died.
According to the CDC, influenza and pneumonia together caused 55,000 deaths in the U.S. in 2017.
Given the scientific evidence that Covid-19 is highly contagious, let’s do a Pareto Distribution (80/20 rule) projection and estimate that 20% of the the U.S. population gets Covid-19. That’s 66 million people, roughly 50% higher than the 45 million who catch a flu virus in a “bad flu” season.
Data suggests between 2% and 3.4% of all Covid-19 cases end in death, but the deaths are concentrated in the 20% of cases that become severe, and in the vulnerable populations within the 20% severe cases that require hospitalization.
Using the lower CFR (case-fatality rate) rate, 2% of 66 million is 1.3 million, so if Covid-19 infects only 20% of the U.S. populace, current data suggests 1.3 million people will die. This is considerably more than 24,600,or 55,000. (Total annual deaths in the U.S. are around 2.8 million.)
But these mortality data are drawn from small numbers of patients who have had access to intensive care. Anecdotal evidence from places where the healthcare system has been overwhelmed (Wuhan) so intensive care is unavailable to the majority of severely ill patients suggest much higher death rates around 15%, with worst-case scenarios going as high as 80% mortality for untreated severe cases in vulnerable populations (elderly and chronically ill).
If 20% of all cases can be expected to be severe and require hospitalization/intensive care (20% of 66 million is 13 million people), then intensive care will quickly become unavailable due to the low number of intensive care beds in the U.S. (94,000). The total number of all hospital beds in the U.S. is around 931,000. (Recall that the majority of these beds are already in use, so the number available to those severely ill with Covid-19 is a fraction of the total.)
If 15% of untreated severely ill patients die, that is 13 million X 15% = 1.95 million.
So let’s cut all these numbers in half: let’s assume only 10% of the U.S. populace gets the Covid-19 virus (33 million), so only 6.6 million people become severely ill. If 15% of untreated severely ill patients eventually die, that’s 1 million deaths in the U.S. alone.
In other words, the death rate is only low if the number of severely ill patients remains very low. Once the number of patients needing hospitalization exceeds the number of ICU beds, the death rate leaps dramatically.
All this assumes there are not already more lethal variants in some human populations, and it also ignores the issue of re-infection: A tour guide in Japan tested positive for the coronavirus for a 2nd time, less than a month after recovering.
Authorities are well aware of the potential for the Covid-19 to spread rapidly and cause a great many deaths. But they’re also concerned about the consequences of an economic crash as people avoid public places (i.e. “social distancing”) as the most effective preventative measure to reduce the chances of contracting the virus.
The resulting layoffs and business closures will trigger financial and economic consequences that may not be recoverable if these trends self-reinforce (more layoffs cause consumption to decline, triggering more layoffs, etc.).
I wrote about this on February 11: China’s Fatal Dilemma.
If authorities downplay the Covid-19 pandemic and encourage people to continue flying, gathering in public, etc. in order to keep the economy humming, that will accelerate the spread of the virus.
When people awaken to the dangers of the pandemic (for example, when ICU beds are all filled and severely ill patients are being turned away), they will panic and pursue “social distancing” regardless of what officials say. When complacency gives way to panic (yes, it can happen here and yes, it can happen to you), the economy will crash.
In other words, the economy will crash either way: if authorities force “social distancing” to limit the spread of the virus or if they downplay the pandemic and let the virus spread to the point that people panic and “socially distance” themselves regardless of official entreaties to get out there and buy, buy, buy.
Forcing “social distancing” won’t stop the eventual spread of the virus, because as soon as restrictions are eased the virus will enter the newly open cities via asymptomatic carriers and a second wave of infections will spread. Forcing “social distancing” while thousands of airline flights and railway travel continue to spread asymptomatic carriers to every transportation node on the planet is not going to stop the spread of the virus.
The science suggests a significant percentage of the human populace will eventually get the Covid-19 virus. Estimates run from 40% to 70%; You’re Likely to Get the Coronavirus (The Atlantic).
Common sense suggests complacency is misplaced, and efforts should be made to minimize the risk of getting the virus until a reliable vaccine is available, which those with experience in the field suggest might be a year or 18 months away.
The science is telling us that the global economy will experience a depression as these realities sink in. Authorities pushing complacency as a short-term financial panacea are doing an enormous disservice to the people who entrusted them with power. The more effective strategy would be to prepare to deal with a global depression while limiting the spread of the virus by whatever means are available, which at present boils down to social distancing and increased hygiene.
Here is an example of status quo complacency in the U.S.: the person returns from Japan with symptoms of Covid-19, tests negative for conventional flu and other viruses, CDC refuses to test for Covid-19, no special protocols despite the obvious risk of Covid-19, staff tells the patient to go home by whatever transport he/she normally uses. My COVID-19 Story. Brooklyn. (via Maoxian)
So either the science is wrong and the complacent will be proven correct, or the science is correct and the complacent will be wrong.